Episode Details
Back to Episodes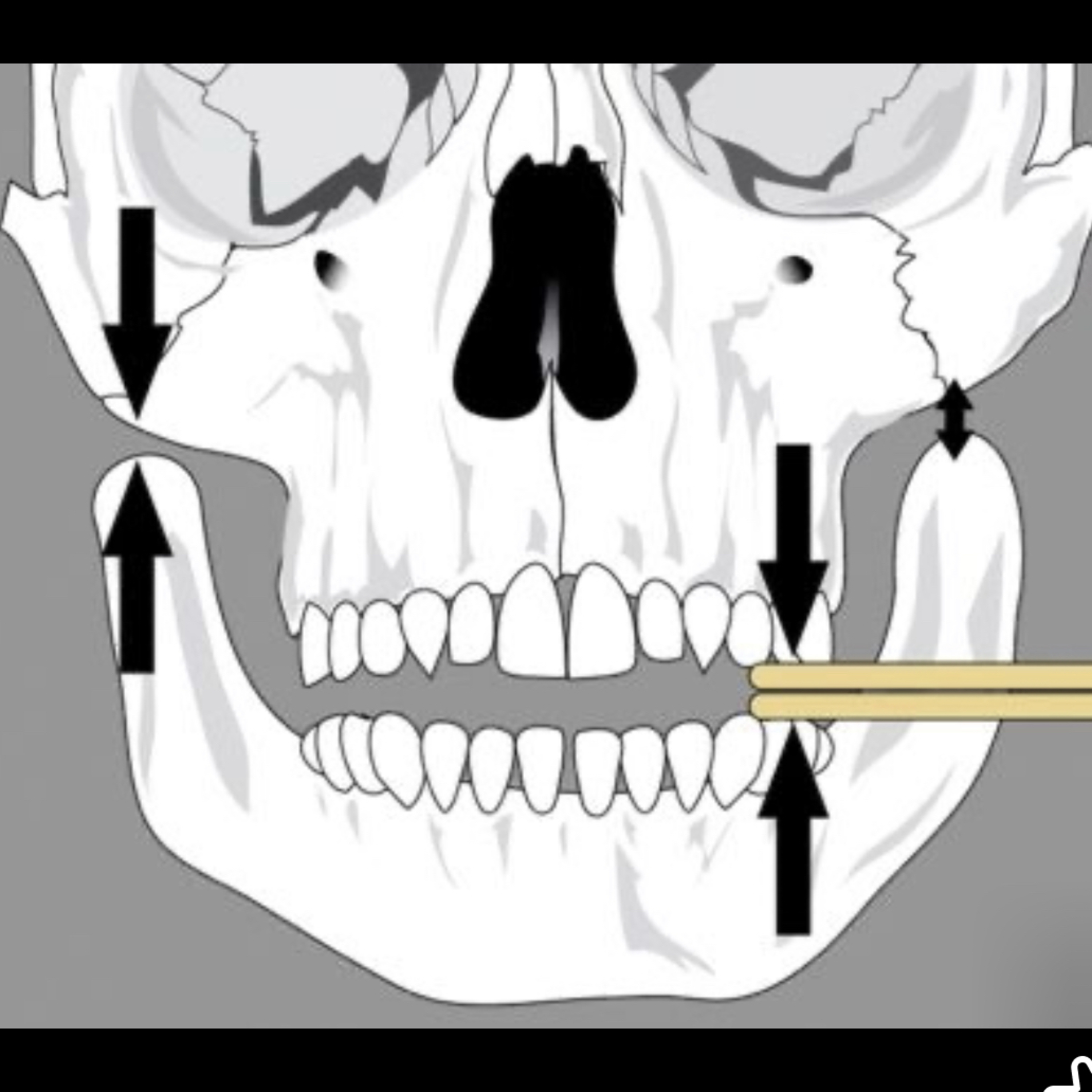
📝 “What is TMJ Loading?”
Description
- 1.8.25
Quick Review #262 - #dental #dentist #dentistry #dentalstudent #dentalschool #teeth #cavity #wisdomteeth #extraction #oralsurgery #oralsurgeon #implant #implants #dentalimplant #dentalimplants #TMJ
TMJ loading refers to the process of applying mechanical stress or forces to the temporomandibular joint (TMJ), which connects the mandible (lower jaw) to the temporal bone of the skull. This loading can occur physiologically during normal activities, such as chewing, speaking, and swallowing, or pathologically in conditions that stress the joint.
Types of TMJ Loading
1. Static Loading: Prolonged application of pressure without movement, such as clenching or bruxism (teeth grinding).
2. Dynamic Loading: Repeated application of force with movement, as in chewing or other mandibular motions.
Physiological TMJ Loading
• Normal TMJ loading occurs during activities like mastication (chewing), where the joint is subjected to cyclic compressive and tensile forces. This loading is critical for maintaining the health of the joint’s cartilage, synovial fluid, and surrounding structures.
Pathological TMJ Loading
Excessive or abnormal loading can contribute to TMJ disorders (TMD). Examples include:
• Bruxism: Chronic clenching or grinding can lead to joint and muscle strain.
• Malocclusion: Misaligned teeth can cause uneven forces on the TMJ.
• Trauma: Acute injuries may overload the joint structures.
Effects of TMJ Loading
1. Biomechanical Changes: Excessive or uneven loading can wear down the articular cartilage, leading to degenerative joint diseases such as osteoarthritis.
2. Inflammation: Pathological loading can trigger inflammation of the synovium, resulting in pain and reduced mobility.
3. Muscular Strain: Abnormal loading affects surrounding muscles, contributing to tension and discomfort.
Diagnostic Relevance
Evaluating TMJ loading is critical in diagnosing TMD. Clinicians assess:
• Bite forces and occlusal contacts.
• Range of motion and joint sounds.
• Pain patterns during static and dynamic activities.
References:
1. Lövgren, A., Visscher, C. M., Alstergren, P., Lobbezoo, F., Häggman-Henrikson, B., & Wänman, A. (2020). The outcome of a temporomandibular joint compression test for the diagnosis of arthralgia is confounded by concurrent myalgia. Clinical Oral Investigations, 24(1), 97–102. https://lnkd.in/ew3ciWev.
2. Okeson, J. P. (2019). Management of Temporomandibular Disorders and Occlusion (8th ed.). Elsevier.
3. Manfredini, D., Castroflorio, T., Perinetti, G., & Guarda-Nardini, L. (2013). Retrusive overjet as a risk factor for temporomandibular joint disk displacement: A systematic review and meta-analysis. Journal of Orofacial Pain, 27(2), 121-129.
4. Tanaka, E., & Tanne, K. (2005). Biomechanics of the temporomandibular joint. Journal of Oral Biosciences, 47(3), 155-161
5. ChatGPT 2025
#podcast #dentalpodcast #doctorgallagherpodcast #doctorgallagherspodcast #doctor #dentist #dentistry #oralsurgery #dental #dentalschool #dentalstudent #doctorlife #dentistlife #oralsurgeon #doctorgallagher