Episode Details
Back to Episodes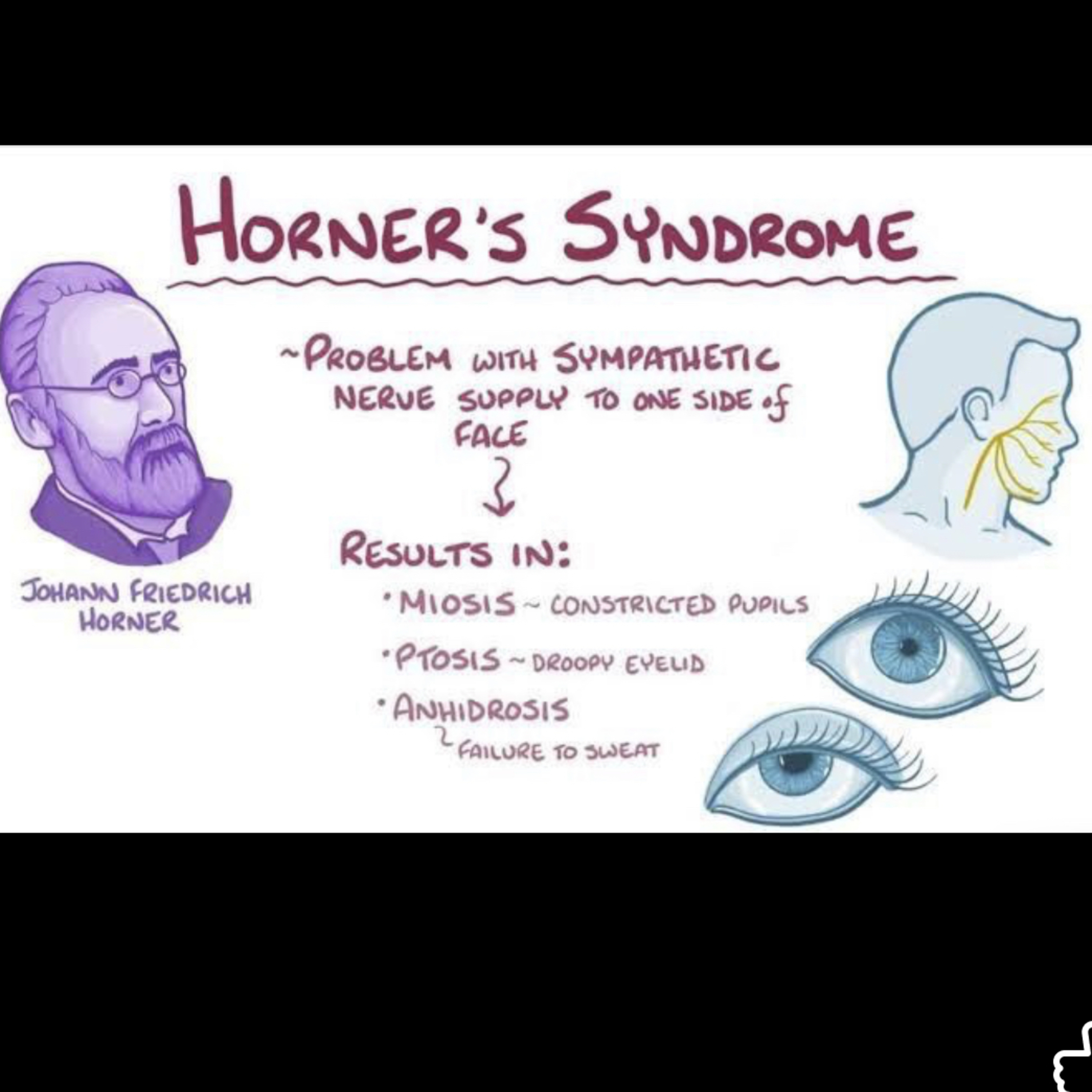
📝 “What are the Differences Between Horner’s & Frey Syndrome?”
Description
- 12.24.24
Quick Review #258 - #pathology #oralpathology #doctorgallagher #oralsurgery #oralsurgeon #dentist #dentistry #dental
Horner’s Syndrome - A neurological disorder caused by disruption of the sympathetic nerve pathway to the face.
Key Features (Oral Signs/Symptoms):
1. Anhidrosis (lack of sweating):
• Reduced or absent sweating on one side of the face (including oral mucosa if involved).
• No direct oral implications, but dryness may lead to discomfort.
2. Ptosis (drooping eyelid):
• No direct oral impact but can indicate autonomic nerve dysfunction affecting nearby areas.
3. Miosis (pupil constriction):
• No direct dental relevance, though it may indicate deeper sympathetic system involvement.
4. Vasodilation and Enophthalmos (retraction of the eyeball):
• Changes in vascular tone may theoretically affect gingival or mucosal blood flow on the affected side.
5. Underlying Causes:
• Can arise secondary to conditions like apical lung tumors, carotid artery dissection, or neck trauma, which may also cause referred pain in the jaw or neck
Frey Syndrome (Auriculotemporal Syndrome) - A condition characterized by sweating and flushing of the skin over the parotid gland region, triggered by eating, due to aberrant regrowth of parasympathetic nerve fibers following injury.
Key Features (Oral Signs/Symptoms):
1. Gustatory Sweating:
• Sweating occurs in the cheek and preauricular area during eating or thinking about food.
• No direct oral signs, but the patient may notice unusual sweating when consuming specific foods.
2. Facial Flushing:
• Flushing can extend to the cheek and skin overlying the parotid gland when eating.
3. Parotid Gland Trauma or Surgery:
• Often follows parotidectomy, abscess drainage, or facial trauma.
• If post-surgical, there may be associated scars or swelling near the oral cavity/parotid region.
4. Trigger:
• Typically triggered by mastication or salivation, linking the condition to oral function.
5. Management:
• Botulinum toxin injections into the affected skin or dietary modifications to avoid triggering foods
References:
1. Hunain. (n.d.). Horner’s Syndrome [Illustration]. Retrieved December 23, 2024, from https://lnkd.in/ekvYfMN4
2. Gross, N. D., & Wax, M. K. (2020). Auriculotemporal Syndrome (Frey Syndrome): Diagnosis and Management. Otolaryngologic Clinics of North America, 53(5), 975–982.
3. Loewenfeld, I. E. (1993). The Pupil: Anatomy, Physiology, and Clinical Applications (Vol. 1). Butterworth-Heinemann.
4. Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2016). Oral and Maxillofacial Pathology (4th ed.). Elsevier.
5. ChatGPT. 2024.
#podcast #podcasts #dentalpodcast #dentalpodcasts #doctorgallagherpodcast #doctorgallagherspodcast #doctor #dentistry #oralsurgery #dental #viral #dentalschool #dentalstudent #omfs #surgeon #doctorlife #dentistlife #residency #oralsurgeon #dentist #doctorgallagher